Is Modern Medicine Dismissing Opportunities to Prevent Breast Cancer?
The journey from health to disease is a time continuum along which many points could be identified. Thermography, with its non-radiation, non-contact and low-cost basis has been clearly demonstrated to be a valuable and safe early risk marker of breast pathology, and an excellent case management tool for the ongoing monitoring and treatment of breast disease when used under carefully controlled clinical protocols.
Thermography is a test of physiology and therefore complementary to and not competitive with structural breast testing such as mammography, ultrasound or MRI. With DITI, subtle physiological changes can be closely monitored, providing feedback for doctors and patients who seek to be more proactive with breast health protocols.
Thermography can detect subtle physiological activity that may accompany pathology and offers the ability to evaluate and closely monitor:
• Early risk markers
• Fibrocystic changes
• Hormonal changes
• Vascular changes
• Lymphatic congestion
• Paget’s disease
• Mastitis and more
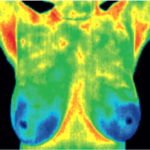
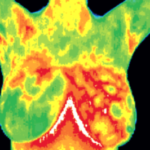
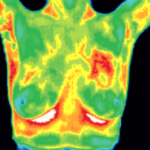
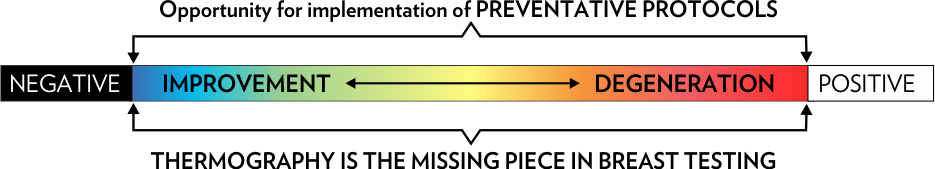
Thermography is Safe and Beneficial for Younger Women
DITI is especially appropriate for younger women between 30 & 50 whose denser breast tissue makes it more difficult for mammography to pick up suspicious lesions. This test can provide a ‘clinical marker’ to the doctor, mammographer or sonographer that a specific area of the breast needs particularly close examination.
| AGE | AVERAGE TUMOR DOUBLING TIME |
| Under 50 | 80 days |
| Age 50 - 70 | 157 days |
| Over age 70 | 188 days |
Source: Cancer 71:3547-3551, 1993
Breast cancers tend to grow significantly faster in women under 50. The faster a malignant tumor grows, the more Infrared radiation it generates. For younger women in particular, results from DITI screening can lead to earlier detection and, ultimately, longer life.
Increase your chances of detecting breast cancer in its earliest stages by understanding the need for, and participating in an early detection program.
The Value of Post Cancer Diagnosis Thermographic Evaluation...
Thermography can be used post treatment to establish a new physiological baseline and closely monitor even subtle physiological changes with annual or semi-annual exams to evaluate the need for additional testing or more proactive protocols to improve breast and lymphatic system health.
Breast Thermography - Screening and Imaging Procedure
There is no contact, no radiation and no contrast agents are used. The room temperature will be cool and you will be seated in front of the thermal camera for imaging. At Be Well Thermal Imaging, the imaging will be performed by a female Certified Clinical Thermographer.
Prior to breast imaging you will be asked to disrobe from the waist up and a gown will be provided for you to wear while you recline or lie on a cooling bed and the thermographer goes over your history and notes with you. Time will be allowed both before and during the exam for your skin's surface temperature to equilibrate. Once the areas being imaged have cooled, the thermographer will have you move to a seat in front of the camera. You will disrobe and place your hands on the top of your head for breast imaging. Please let your thermographer know if you have any limitations with raising your hands above your shoulders.
The thermographer will use a computer program to take images of your breasts to obtain six images including front, back, lateral and oblique views to submit to EMI (Electronic Medical Interpretation) where doctors called thermologists will interpret them and draw a report that will be returned to you electronically and/or via mail.
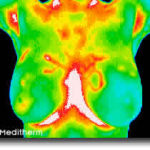
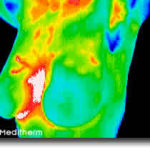
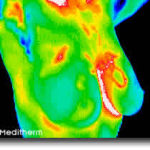
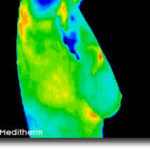
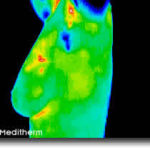
Your initial breast imaging study will require an extra 15-20 minutes for the thermographer to take a complete history and notes about your specific complaints or concerns, so please allow 45-60 minutes for the first appointment. Your followup breast thermography exams (thermograms) will only take about 25 minutes.
Thermography is a test of physiology so comparison studies are important to the effectiveness of this type of breast screening. You will need to establish a stable baseline before continuing with annual tests. This is done by having two thermograms compared. Optimally, the two baseline studies should be done three months apart. A stable baseline is established when two consecutive studies are compared and exhibit no changes in thermal patterns. After your baseline is established, future studies will be compared back to the baseline and to previous studies in your history. These comparisons help monitor the stability or changes in your breast physiology over time.
Be Well Thermal Imaging performs thermography in Naples, FL, but because we participate in the Meditherm system, subsequent comparison studies can be facilitated worldwide. If you are no longer in Naples, just follow up with another ACCT (American College of Clinical Thermology) approved thermographer to continue your breast screening program wherever you go.
You are welcome to bring a companion or partner to be present at the examination. Please read "How to prepare for your Thermogram" before you schedule so you will know what activities to avoid that day.

Thermal Imaging is Ideal for:
- Women with breast implants
- Young women with family history
- Women of any age who want to reduce their exposure to radiation
Thermography's role in breast cancer and other breast disorders...
is to help in early detection and monitoring of abnormal physiology and the establishment of risk factors for the development or existence of cancer. When used with other procedures the best possible evaluation of breast health is made.
This test is designed to improve chances for detecting fast-growing, active tumors in the intervals between mammographic screenings or when mammography is not indicated by screening guidelines such as for women under 50 years of age.
Thermography demonstrates heat patterns that are strongly indicative of breast abnormality; the test can detect subtle changes in breast temperature that indicate a variety of breast diseases and abnormalities and once abnormal heat patterns are detected in the breast, follow-up procedures including mammography may be necessary to rule out or properly diagnose cancer and a host of other breast diseases such as fibrocystic syndrome, Pagets disease, etc.
Canadian researchers found that infrared imaging of breast cancers could detect minute temperature variations related to blood flow and demonstrate abnormal patterns associated with the progression of tumors. These images or thermograms of the breast were positive for 83% of breast cancers compared to 61% for clinical breast examination alone and 84% for mammography.
By performing thermography years before conventional mammography, a selected patient population at risk can be monitored more carefully, and then by accurately utilize mammography or ultrasound as soon as is possible to detect the actual lesion - (once it has grown large enough and dense enough to be seen on mammographic film), can increase the patients treatment options and ultimately improve the outcome.
It is in this role that breast screening with thermal imaging provides its most practical benefit to the general public and to the medical profession. It is certainly an adjunct to the appropriate usage of mammography and not a competitor. In fact, thermography has the ability to identify patients at the highest risk and actually increase the effective usage of mammographic imaging procedures. While participation in a DITI early detection program can increase your chance of detecting and monitoring breast disease, as with all other tests, it is still not a 100% guarantee of detection.
Thermography, with its non-radiation, non-contact and low-cost basis has been clearly demonstrated to be a valuable and safe early risk marker of breast pathology, and an excellent case management tool for the ongoing monitoring and treatment of breast disease when used under carefully controlled clinical protocols.
HOW TO PREPARE
Please click here for instructions on how to prepare for your thermography appointment.
BOOK AN APPOINTMENT
Click here to schedule thermography in Naples via the Be Well Thermal Imaging appointment tool.



